A SIMPLIFIED UNDERSTANDING OF LOW
BACK PAIN
Lyn Lampman, M.R.T.
"My aching back!"
How many physicians have heard this phrase in their practices?
It is estimated
that 75% of people of all ages and walks of life experience back pain at
some point in their lives and that this problem accounts for 15% of sick
leaves. It is one of the most common complaints heard by today's
physicians, affecting rich or poor and working or non-working classes.
Since we live in a society where we tend to sit all day in an office, commute
to work by car and have little or no time for exercise, we are easy victims
for low back pain. After spending the past twenty years running a
private x-ray clinic for orthopaedic surgeons, I will try in this article
to help you understand the different diagnosis and treatments for this
problem without going to into a great deal of complicated jargon.
The causes of
low back pain are many and varied as are the means of diagnosis and treatment.
Low back pain is a symptom
not a disease. Therefore, a certain degree
of pessimism and fear often prevents the patients from seeking medical
care. Unfortunately, some physicians, confronted with conflicting reports
and multiple diagnostic and therapeutic methods, may themselves be pessimistic
on how to treat low back pain problems.
With todays
advances in medicine most patients can be diagnosed, treated and with proper
care return to normal activities. The good news is that in the vast
majority of these people, probably greater than 90% will recover completely
without surgical treatments, only 2-3% of people with back pain will have
a herniated disc and about 1% will have compression of a nerve root.
The evaluation
of back pain requires a physician experienced in this specialty.
The workup begins with a detailed history and physical examination. The
specialist will ask about the quality of the pain, where it radiates, factors
that worsen or alleviate the pain and other related questions. The physical
examination concentrates on motor and sensory function. Radiographic
evaluation may be indicated, usually starting with a set of plain X-rays.
Over the years, I have x-rayed patients with severe low back pain only
to discover a gallbladder full of stones. Removal of the gallbladder
in some of these cases alleviated the pain. If your physician is
suspicious of a structural lesion, based on the history and examination,
one or more of the following additional studies may be performed:
Anatomy
The back is
a chain of blocks (the vertebrae) stacked one on the other and kept from
collapsing by an exact system of muscles and ligaments that act with synergistic
(co-operative) and antagonistic (opposing) precision. It completely encloses
and protects the spinal column, acts as a flexible support to the trunk
and as a central axis of limb movement. Thirty-three spinal vertebrae are
held together by multiple ligaments and interposed cartilages: 7 cervical,
12 thoracic, 5 lumbar, 5 sacral (fused into one) and 4 coccygeal (often
fused into one). The vertebrae of each group have features that distinguish
them from the vertebrae of the other groups. No two vertebrae are
exactly the same and each is modified so that its position in the spine
can be recognized. A developing fetus, you have probably noticed, develops
with a forward curve (kyphotic) in the womb. Shortly after birth,
the spine develops its normal cervical and lumbar lordoses with compensatory
thoracic and sacral kyphoses.
Since low back
pain usually stems from problems affecting the lumbar vertebrae and sacrum,
this discussion will give primary emphasis to the lumbosacral area.
The lumbar vertebrae are large and massive
because of their weight-bearing functions. AP views of the lumbar area
show the body, laminae, spinous processes, transverse processes and the
intervertebral disc spaces. The lateral view demonstrates the bodies, disc
spaces and intervertebral foramina, intervertebral joints and the spinous
processes. Oblique views of the lumbosacral junction are sometimes required
for the demonstration of the part of the neural arch between the superior
and inferior articular processes.
Classification
and Different Diagnosis
-
Mechanical Back Pain
-
Degenerative Disorders
-
Congenital Disorders
-
Sciatica
-
Herniated Disc
-
Spinal Stenosis (Spondylosis)
-
Spondylolysis & Spondylolisthesis
-
Trauma
Mechanical
Back Pain
Also known as
a "back strain". The diagnosis excludes anatomic sources of origin such
as disc herniation, spondylosis, etc. The causes may be multifactoral,
including strain of the muscles of along the spine, strain of ligaments
of the spine, degenerative facet joint disease (the joints between the
bones of the spine) or others. Poor muscle tone is a common cause of muscle
strains and ligament sprains. When hip pathology is suspected (e.g.-osteoarthritis
or necrosis) hip x-rays can assist the diagnosis. Lumbar scoliosis in adolescence
can later cause severe back pain when the patient reaches adulthood.
Degenerative
Disorders
Osteoarthritis
is a wear and tear problem and is associated with degenerative changes
in the articular cartilage. In the vertebral column, the facet joints are
involved. Repeat trauma, such as excessive and strenuous exercise pursuits
during the teen years, plays a role but doesn't completely explain the
disease. Heredity and obesity contribute to the etiology. It is well known
that the human spine begins to "squeak & rattle" with increased trauma,
obesity and age. The following example shows degeneration of the intervertebral
discs with changes at the vertebral margins and osteophyte (spur) formation.
Notice the narrowing of the disc space.

Congenital
Disorders
Minor anomalies
of the vertebrae are so common that a variation from "the norm" is not
always considered the cause of back pain. A change in the number of vertebrae
in the lumbar spine is the most significant congenital anomaly that can
cause low back pain. Lumbarization of the first sacral vertebral
gives the patient individual six lumbar vertebrae and causes a greater
stress on the lumbosacral joint. Sacralization of the fifth lumbar
vertebra, which results in four lumbar vertebrae, is unlikely to cause
symptoms when the entire vertebra is incorporated into the sacrum. The
most common form of sacralization is for one of the transverse processes
of the fifth to be enlarged and joined to the sacrum. This may cause strain
on the side opposite the sacralization.
Sciatica
This is described
as pain radiating into the buttock, back of the thigh and often into the
calf and foot. It is usually caused by irritation of a sciatic nerve root,
often from compression by a disc or degenerative disease.
Herniated Disc
Also known as
herniated nucleus pulposus, disc rupture or disc prolapse. Ruptured discs
are among the most common and painful of all back ailments. The intervertebral
discs are cartilaginous plates, surrounded by a fibrous ring, that lie
between the vertebral bodies and serve to cushion them. Through degeneration,
wear and tear or trauma the fibrous tissue (annulus fibrosus) constraining
the soft disc material (nucleus pulposus) may tear. This results in protrusion
of the disc or even extrusion of disc material into the spinal canal or
neural foramen. In addition, the motor fibers of the affected root are
also compressed and this situation leads to atrophy and weakness in the
appropriate muscles. This is known as a herniated, ruptured or prolapsed
disc. The most common complaint in patients with a herniated disc is that
of severe low back pain developing immediately or within a few hours after
an injury. Often the patient (usually between the ages of thirty and fifty
years) tells of heavy lifting or a twisting motion while moving a heavy
object. The pain, accentuated by forward bending, sneezing or straining,
is associated with severe muscle spasm. There is flattening of the lumbar
area from loss of the normal lumbar lordosis.
The disc herniation
may become significant if a nerve root is compressed. Irritation of the
nerve root produces pain in the distribution of that nerve. Different
levels of nerve root compression cause different symptoms. Compression
of the nerve root at L4&5 causes pain over the sacroiliac joint and
the lateral thigh and leg with difficulty walking on heels. Whereas a compression
of the nerve root at L5S1 causes pain over the sacroiliac joint, hip, back
and lateral side of leg down to the heel with difficulty walking on toes.
For this reason, a herniated lumbar disc normally produces sciatica but
not the back pain per se. If sensory function of the impinged nerve root
is impaired, numbness will result, the exact area determined by the particular
root.
The actual amount
of disability from a disc depends on several mechanical factors:
-
How much disc material has entered the neural
canal
-
How many nerve roots have been compressed
-
How much space exists inside the neural canal
For
example, some patients have a very narrow canal so even a small herniation
will cause severe symptoms whereas others may have a large canal so a small
herniation will have little effect.
Diagnosis should
be suspected from the history and physical examination. Radiographic studies
should be done to make a define diagnoses and define its location. It is
impossible to diagnose disc protrusion by simple X-rays. Generally an MRI
provides excellent detail. A CT scan, while inferior to MRI in soft tissue
detail, is superior in bony detail and faster and less expensive. A good
quality CT is often sufficient in an uncomplicated herniated lumbar disc.
A myelogram with a CT gives excellent definition of the spaces around the
nerve roots but its disadvantage is the injection of contrast dye through
a lumbar puncture.
The mainstay of therapy for a herniated
lumbar disc is conservative treatment, that is, nonsurgical. In the majority
of patients the symptoms resolve or subside to a level allowing normal
activity within two to three weeks. If rest with limited activities fails,
surgery may be considered.
Surgery for
removal of a herniated lumbar disc has been one of the most commonly performed
procedures. Up until the past 5 years or so, the procedure has been fairly
standard. An incision is made vertically along the midline of the back,
usually about 2 inches long. Some of the muscles overlying the bone (lamina)
that forms the back of the spinal canal are separated off the bone. A small
window is drilled in the laminae overlying the herniation. The nerve root
is identified and gently retracted away to expose the offending herniation.
The disc material is then removed and the wound is closed in a way that
restores the normal anatomic layers.
Postoperative
recovery is relatively short. Patients are walking the same night or the
next morning and discharged home in three or four days. The recovery period
is about six to eight weeks. The vast majority of patients experience permanent
relief of pain. Recovery of motor function is variable.
Nowadays, a
new endoscopic procedure referred to as MicroEndoscopic Discectomy (MED)
significantly reduces hospital stays and recovery time for many people
suffering from herniated discs. The objective is to decompress the nerve
root. Approximately 75% of patients with herniated discs are candidates
for this procedure. The surgery can be performed on an outpatient basis.
The MED procedure uses microsurgical and endoscopic techniques with advanced
optical systems. Instruments are inserted into the back through a tube
slightly larger than a fountain pen. Doctors perform the surgery while
viewing a video monitor. The procedure is less painful, requires only a
half inch incision and patients are back at work within seven to ten days.
The success rate: 93% excellent, 7% good. The only drawback is not that
many hospitals are equipped with the MED system.
Lumbar Stenosis
(Spondylosis)
The term lumbar
stenosis refers to any narrowing of the spinal canal. The most common cause
is degenerative, occurring with aging in essentially the entire population.
The degenerative narrowing is referred to as spondylosis. This is
a complex problem requiring an individualized approach for each patient,
by an experienced specialist. Another cause of stenosis is the slippage
of one vertebra on another with disalignment and causing narrowing of the
canal. This slippage is called spondylolisthesis that will be dealt
with at a later point.
Several factors
contribute to the narrowing of the spinal canal with degenerative changes.
Arthritis often causes spondylosis so it is often seen in older patients.
First, wear and tear causes the joints (facets) to hypertrophy. This may
be analogous to degeneration and swelling of other joints in the body.
Second, the major ligament of the spinal canal undergoes hypertrophy and
buckling. Third, the intervertebral disc may bulge or herniate. Fourth,
as mention previously, the vertebrae may slip forward. Finally these changes
may be superimposed on a congenitally narrow canal.
Spondylolysis
& Spondylolisthesis
Spondylolysis
is a defect in the isthmus (pars inarticularis) that is the supporting
structure of the vertebra. This can have many causes including degeneration,
trauma and congenital defects. Spondylolisthesis is a defect in both sides
of the vertebra through the pars, with anterior slipping of the vertebral
body. The slippage is classified from grade I to IV. A grade I spondylolisthesis
means displacement up to 25% and a grade IV slip means a complete forward
displacement of the affected vertebral body. The fifth lumbar vertebra
is most commonly affected followed in frequency by the fourth vertebra.
Symptoms usually come from the spinal nerves that may be pinched as the
vertebra slips forward. While both spondylolysis and spondylolisthesis
can be congenital most cases are acquired and repeated stress is considered
to be the cause.
Oblique x-rays
of the lumbosacral spine demonstrate pictures characteristic of each condition.
For example, on an oblique x-ray, a normal vertebra gives the appearance
of a "Scotty dog". If the "Scotty dog" is wearing a collar, there is a
defect in the pars interarticularis and the patient has spondylolysis.
If the head of the "Scotty dog" is separated from the neck, the patient
has spondylolisthesis.

Posterior oblique
view demonstrating formation of radiographic "Scotty dog". On left side
from top to bottom:
-
Superior articular process (ear of "Scotty dog")
-
Pedicle (eye)
-
Transverse process (head)
-
Isthmus (neck)
-
Spinous process and Lamina (body)
-
Inferior articular process (foreleg)
-
Opposite Inferior articular process (hindleg)
In
simple spondylolysis, on the left, the dog appears to be wearing a collar.
In spondylolisthesis, on the right, the dog appears decapitated.
Trauma is the
most frequent cause of back pain. Every day people injure their backs because
of foolish lifting practices, a fall, an athletic injury or a possible
MVA. The main reason for the majority of these injuries is that so many
people are in poor physical condition. Most muscle strains and back pain
could be avoided by proper weight control and daily exercise to keep trim
and retain good muscle tone. Most people, as they pass thirty years of
age, become physically sluggish, gain weight and exercise sporadically,
if at all. When they do, "common sense" is not very common and exercise
is often a strenuous workout at a strenuous sport. Low back pain is also
very common in pregnant women with excessive weight gain who fail to recondition
themselves after delivery. They develop poor muscle tone, obesity, and
spinal decompensation leading to chronic pain.
Compression
fractures usually result from a fall and generally affect the lower thoracic
and upper lumbar area. They are easily diagnosed on an x-ray by their wedge-shaped
appearance and seem to respond well to bed rest. However, if the patient
is osteoporotic the trauma needed to fracture a vertebra is sometimes very
trivial-a minor slip or fall, etc. Therefore, middle-aged and upward patients,
women being more prevalent, account for a great majority of compression
fractures.
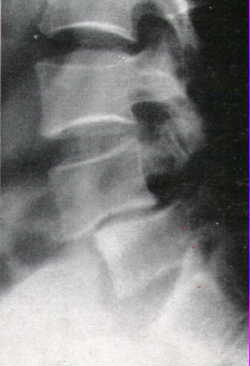
Fracture dislocation
Summary
In this article
I have briefly touched upon the various mechanisms and causes of low back
pain in the hope that the information I have related to you will be easy
to understand and beneficial to family, friends and technicians in the
approach to the patient with low back pain. There are, of course, more
serious problems, a lot more complicated that what my article has dealt
with. You have probably in your own practice seen the insertion of certain
types of hardware because of the major advances in back surgery over the
past five to ten years. The reasoning behind this type of surgery is more
appropriately dealt with by the specialists in order that there is no misinterpretation.
As mentioned previously, with modern diagnostic methods and the skills
of today's physicians and surgeons, a great number of these people can
be effectively treated to lead relatively normal lives.
Illustrations thanks to Dr. Frank H. Netter.
M.D.

This site was lasted
updated April 25/09
Sign
My Guest book View
My Guest book
View
My Guest book
Comments
Welcome




![]()
