*Division of Gynecologic Oncology, Department of Obstetrics and Gynecology, University of California at Irvine--Medical Center, 101 The City Drive, Orange, California 92868: and **Department of Pathology, Memorial Medical Center, 1400 Atlantic Avenue, Long Beach, California 92806
Advanced-Stage Small Cell Carcinoma of the Ovary in Pregnancy: Long-Term Survival after Surgical Debulking and Multiagent Chemotherapy
Krishnansu Tewari, M.D.,* Cheryl Brewer, M.D.,* Fabio Cappuccini, M.D.,* Cynthia Macri, M.D.,*
Lowell W. Rogers, M.D.,** and Michael L. Berman, M.D.*
We report the longest disease-free survival achieved in an advanced-stage small cell carcinoma of the ovary. The patient had a stage IIIc tumor diagnosed during pregnancy. She underwent a total abdominal hysterectomy, bilateral salpingo-oophorectomy, omentectomy, and optimal tumor debulking. Following her immediate postoperative recovery, she was treated with a multiagent chemotherapy regimen with germ cell activity consisting of vinblastine, cisplatin, cyclophosphamide, bleomycin, doxorubicin, and etoposide. She is alive and without evidence of disease 5˝ years after diagnosis. This is the second reported case in pregnancy and the longest disease-free survivor of metastatic small cell ovarian carcinoma in the medical literature. 1997 Academic Press
INTRODUCTION
Small cell carcinoma of the ovary is a rare tumor usually affecting children and young women. Although the tumor has some histologic features consistent with an epithelial origin, some of the histologic features as well as immunohistochemical and ultrastructural evidence support a germ cell origin [1,2]. The propensity to occur unilaterally in young women also suggests a possible germ cell origin. Small cell ovarian cancer usually manifests as a solid or mixed cystic and solid tumor with a prediliction for widespread intra-abdominal metastases. It is associated with hypercalcemia in nearly two-thirds of cases and may secrete a variety of tumor markers frequently associated with some of the germ cell tumors [2,3].
Historically, the prognosis for patients with this disease has been extremely poor. However, in recent years, objective responses have been obtained with aggressive multiagent chemotherapy including drugs with germ cell activity. We report what we believe to be the first 5-year survival of a patient presenting with advanced-stage small cell ovarian cancer. She was treated with six courses of a multiagent chemotherapeutic regimen consisting of vinblastine, cisplatin, cyclophosphamide. bleomycin, doxorubicin, and etoposide (VPCBAE) following optimal tumor resection.
CASE REPORT
M.B. is a 26-year-old. previously healthy, black, gravida 4, para 3, who presented in April 1991 with abdominal pain at 13 weeks gestation. An ultrasound demonstrated a 12 × 8-cm right adnexal cystic and solid mass for which she underwent exploratory laparotomy and right salpingo-oophorectomy at a community hospital. The histologic findings were initially reported as an undifferentiated carcinoma. She was referred to the Division of Gynecologic Oncology at the University of California at Irvine.
Serum levels of CEA, aFP, and CA-125 were within normal limits. while the qualitative serum BHCG was positive secondary to the pregnancy. The serum calcium was also within the normal range (9.6 mg/dl). In addition, the clinical examination and a chest radiograph were without evidence for metastatic disease.
A review of the histologic material was conducted by R.E. Scully, M.D. of Harvard Medical School and the Massachusetts General Hospital who reported a diagnosis of small cell carcinoma of the ovary. The microscopic description was of a small cell variant, highly anaplastic with numerous mitotic figures. There were some follicle-like spaces present in the neoplasm and the presence of benign-appearing mucinous epithelium on at least one slide (see Fig. 1).
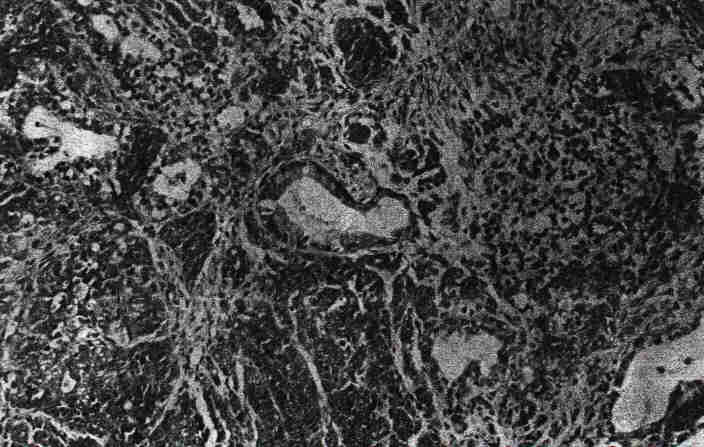
FIG. 1. Ovarian primary, small cell carcinoma. Tumor cells have scant amphopilic cytoplasm and show variable arrangements in sheets, clusters, and cords. Mature mucin-producing epithelium is focally present (center). Scattered irregular follicle-like arrangement of undifferentiated cells are also seen (H & E; original magnification, 200x).
The patient underwent re-exploration, including total abdominal hysterectomy, left salpingo-oophorectomy, omentectomy, and tumor debulking. The surgical findings included a 14-week gravid uterus, small left ovarian cysts, and widespread nodular tumor masses on the surfaces of the pelvic and abdominal peritoneum, small and large bowel and omental surfaces, consislent with FIGO stage IIIc. The patient was optimally debulked with a maximum residual disease of less than 1cm [3]. Pathologic assessment confirmed metastatic small cell carcinoma in the omentum and pelvic peritoneum and on the surfaces of the sigmoid colon and anterior abdominal wall (see Fig. 2). This material was also reviewed by Dr. Scully who confirmed the diagnosis.
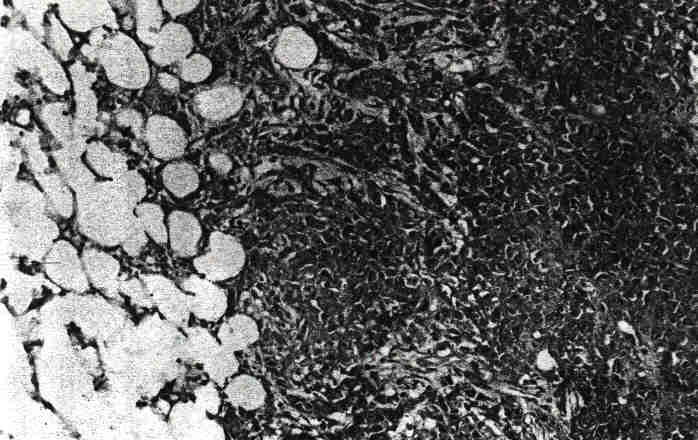
FIG.2. Omental metastasis. Tumor cells invading omental adipose tissue. Mucin-producing epithelium is not present in metatastic deposits (H&E; original magnification, 200x).
The patient had an unremarkable postoperative course and on the eighth postoperative day underwent treatment with the first of six courses of VPCBAE as outlined by Senekjian and co-workers [4]: vinblastine (6 mg/m2) and cisplatin (90 mg/m2) at induction, cyclophosphamide (1 g/m2) and bleomycin (15 U/m2) at 24 hr, and doxorubicin (45 mg/m2) and etoposide (200 mg/m2) at 36 hr (Table I). Due to severe myelosuppression, vinblastine and cyclophosphamide were omitted from the fifth and sixth courses of chemotherapy. She was given granulocyte-monocyte colony-stimulating factor treatments for severe neutropenia during the second, third, and fourth courses of chemotherapy. Although the patient experienced moderate to severe nausea and vomiting and one episode of neutropenic sepsis, she completed six courses of chemotherapy and suffered no long-term sequelae from the regimen.
Table 1
Multiagent Chemotherapy Regimen
| Courses 1-4 | Courses 5-6 |
Induction:
Vinblastine (6 mg/m2)
CIsplatin (90 mg/m2) | Induction:
Cisplatin (90 mg.m2) |
24 hr
BLeomycin (15 U/m2)
Cyclophosphamide (1 g/m2) | 24 hr
Bleomycin (15 U/m2) |
36 hr
Doxorubicin (45 mg/m2)
Etoposide (200 mg/m2) | 36 hr
Doxorubicin (45 mg/m2)
Etoposide (100 mg.m2) |
The treatment regimen in courses 1-4 is as described by Senekjian and co-workers
with the exception that they used doxorubicin at 60 mg/m2 in their report [4].
All drugs were administered via intravenous push with the exception of cisplatin
which was administered intravenously over 2 hr and etoposide
which was administered intravenously over 6 hr.
The patient has been followed radiographically with yearly computerized tomography scans of the abdomen and chest radiographs, all of which have been negative. In addition, clinical examinations and serum tumor markers have been within normal limits. She is currently without evidence of disease 5˝ years after diagnosis.
DISCUSSION
We report the first 5-year survivor who presented with metastatic small cell carcinoma of the ovary. This possible variant of germ cell tumor occurs in younger patients and is generally unilateral. The neoplasm was first reported in 1982 by Dickersin and colleagues in a report of 11 cases associated with hypercalcemia [3]. It has been characterized by a rapidly lethal course despite aggressive therapy, with an overall survival rate of approximately 10% [5]. The few reported survivors have had either early-stage disease or relatively short follow-up, with no reported 5-year survivors who presented with advanced-stage disease [6-9].
In 1987, Ulbright and colleagues provided histologic, immunohistochemical, and ultrastructural evidence suggesting a germ cell origin for small cell carcinoma of the ovary. They postulated that these neoplasms represent a primitive form of germ cell tumor most closely related to the yolk sac tumor [2]. With these findings and the prior reported failure of conventional chemotherapy, in 1989 Senekjian reported five patients treated with a complex chemotherapeutic regimen consisting of VPCBAE [4]. Three patients without measurable disease remained clinically free of disease at the completion of VPCBAE. In addition, two patients who had had measurable disease in the pelvis demonstrated objective responses to chemotherapy. Four patients died of disease between 11 and 18 months after diagnosis, while the fifth patient with stage I disease was alive and free of disease at 29 months of follow-up. Using this six-drug regimen, we have achieved survival in excess of 5 years, the longest reported for an advanced small cell tumor of the ovary.
In 1988, Rasmussen et aL reported the first case of small cell carcinoma of the ovary to be diagnosed in pregnancy [10]. They describe a 22-year-old woman with small cell ovarian cancer without hypercalcemia at 6 weeks gestation discovered at laparotomy for an 11-cm adnexal mass. The pregnancy was continued until the 27th week at which time a cesarean section was performed for severe preeclampsia. There was no evidence of metastatic disease despite multiple biopsies at this time and chemotherapy was not instituted. One year later, the patient recurred and was treated with surgery, chemotherapy, and radiotherapy. She died less than 1 year following recurrence. Her chemotherapy consisted of four courses of etoposide, cisplatin, and bleomycin. This patient represents the only other report of small cell carinoma of the ovary associated with pregnancy.
Because the six-drug combination employed has resulted in the only reported long-term survivor with advanced disease, the VPCBAE regimen should be considered for first-line chemotherapy in the treatment of advanced small cell ovarian cancer. We recognize that individual tumor biology likely plays an important role in determining the response to chemotherapy in this particularly aggressive tumor variant. Institution of chemotherapy early in the disease course may impact positively on survival, while less intensive chemotherapy and delays in onset of therapy should be avoided.
REFERENCES
- Abeler V. Kjorstad KE, Nesland JM: Small cell carcinoma of the ovary. Int J Gynecol Pathol 7:315-329, 1988
- Ulbright TM, Ruth LM, Stehman FB, Talerman A, Senekjian EK: Poorly differentiated (small cell) carcinoma of the ovary in young women: evidence supporting a germ cell origin. Hum Pathol 18: 175-184, 1987
- Dickersin GR, Kline IW, Scully RE: Small cell carcinoma of the ovary with hypercalcemia: a report of eleven cases. Cancer 49:188-197, 1982
- Senekjian EK. Weiser PA, Talerman A, Herbst AL: Vinblasine, cisplatin, cyclophosphamide, bleomycin, doxorubicin and etoposide in the treatment of small cell carcinoma of the ovary. Cancer 64:1183-1187, 1989
- Scully RE, Young RH: Small cell carcinoma of the ovary: a therapeutic challenge. NY State J Med 90:172-173, 1990
- Reed WC: Small cell carcinoma of the ovary with hypercalcemia: report of a case of survival without recurrence 5 years after surgery and chemotherapy. Gynecol Oncol 56:452-455, 1995
- Patsner B, Piver MS, Lele SB, Tsukada Y, Bielat K, Castillo NB: Small cell carcinoma of the ovary: a rapidly lethal tumor occurring in the young. Gynecol Oncol 22:233-239, 1985
- Pruett KM, Gordon AN, Estrada G, Lynch GR: Small cell carcinoma of the ovary: an aggressive epithelial cancer occurring in young patients. Gynecol Oncol 29:365-369, 1988
- Peccatori F, Bonazzi C, Lucchini V, Bratina G, Mangioni C: Primary ovarian small cell carcinoma: four more cases. Gynecol Oncol 49:95-99, 1993
- Rasmussen KL, Jensen ML, Nielsen KM. Velander G: Small cell carcinoma of the ovary diagnosed in early pregnancy. Acta Obstet Gynecol Scand 70:377-379, 1991
Address all correspondence and reprint requests to:
Division of Gynecologic Oncology,
Department of Obstetrics and Gynecology
University of California at lrvine~Medical Center
Clinical Cancer Center, Room 107, Building 23
101 The City Drive
Orange, CA 92868-3298
Fax: (714)456-6463

