

This site provides a window into the 'euthanasia underground'--a secret part of medicine and nursing that few professionals will publicly acknowledge.
I have been involved in extensive medical research and investigation for more than six years. There has been a pattern of consistency throughout my findings and from all the research the facts have begun to emerge. The following information is taken from the medical record of the deceased, Arlene Berry who died suddenly and unexpectedly at the early age of 41, following her admission to the Kirkland and District Hospital on May 23rd of 2000.
The phycicians named herein are currently under criminal investigation for medical homicide and conspiracy to a liability murder.
Some 16 hours after the patient's admission to Kirkland and District Hospital, and less than 5 hours following her transfer to Sudbury Regional Hospital, situated in the City of Sudbury Ontario on May 24th of 2000 the decedent's family were notified by Dr. Stephane Sauve (an Emergency Physician with privileges at the Sudbury Regional Hospital) that Arlene Berry had just died meeting "brain death criteria", in reality she had a clinical condition simulating brain death for which life support was prematurely and wrongfully discontinued due to an unauthorized and unlawful DNR and withdrawal of life support. Although the facts suggest the involvement of a bacterial or possible viral infection, the patient's condition was exacerbated by the drugs and the treatment she received under the care of Drs. Jordan and Spiller at the Kirkland and District Hospital following a combined administration of a major tranquilizer (neuroleptic) and a narcotic, resulting in an intense analgesic and amnesic state of drug-induced paralysis.
Neuroleptanalgesia (neurolept analgesia), also called Conscious Sedation refers to the use of major tranquilisers, ie prochlorperazine/Stemetil in conjunction with narcotics such as morphine (Statex/MS Contin). Patient often gets a `locked-in' state of `outer calm inner panic' that under normal circumstances patients are able to recall vividly and unpleasnantly. The patient is technically awake, but under the influence of the drugs administered. Neuroleptanalgesia requires careful vigilance and monitoring, including pulse oximetry, which in this case was simply ignored to near fatal conclusions, followed by withdrawal of life support.
The "Neuroleptic" effects of the major tranquilisers was first noted by Charpentier. The patient loses interest in their surroundings, emotions are dulled and spontaneous and complex movements are reduced. There is no gross impairment of intelligence and unconditioned or reflex activity remains unimpaired.
Sedation is the common limiting side effect to opioid analgesia and can cause a 'pseudo'-pharmacological ceiling dose. There may be some differences in side effect profiles between different opioids.
Complications have been classified as anaesthetic: inadequate or excessive sedation, pain, nausea or vomiting; respiratory: oxygen saturation <90%, increase in E'CO2 (>6 kPa), hypoventilation (<8 bpm), or airway obstruction; haemodynamic: systolic blood pressure <80 or >170 mm Hg, or heart rate <40 or >110 beats min�1; or neurological: convulsions, brain swelling or development of a new neurological deficit.
Depth of sedation required in many cases is associated with an increased incidence of complications. Over-sedation may also lead to respiratory depression. Any increase in PaCO2 may result in cerebral swelling.
Neurolept analgesia is associated with excessive sedation and a higher incidence of pain and convulsions. Pain triggers autonomic responses that have widespread effects on metabolism, immune function, and the cardiovascular system. The stress produced by pain can lead to hypertension, tachycardia, myocardial ischemia, and myocardial infarction. Fear and pain are frequent adverse effects of many clinical interventions.
Deep sedation is a controlled state of depressed consciousness accompanied by partial loss of protective reflexes, including the inability of a patient to control their airways and the inability to respond appropriately to physical stimulation and verbal command. She was able to wiggle her toes twice in response to verbal request by myself in the presence of a witness.
Arlene Berry's eyes may have been taken by Dr. Sauv�, et al at the Sudbury Regional Hospital upon remote party consent, utilizing deception to obtain that consent, bypassing permission from Arlene Berry's immediate family, ie, de facto (common-law) spouse. Indeed, the fraudulent taking of the patient's eyes would, if this were true, be ultimately seen as a theft. Dr. Sauv� is also a suspect in this medical liability murder and conspiracy, involving several other of his colleagues.
If you take the time to avail yourself of the facts and in particular the links to the overwhelming amount of information and evidence gathered, you will little trouble in making a determination that Arlene Berry came to her demise as a direct result of medical negligence and foul play. This case is now a matter of public record and has been widely reported in the Indymedia IMC, all over Canada, the USA, and in the UK. The long standing silence of the doctors implicated in this homicide infers their active and ongoing concealment. Concealment includes not only secrecy and deception, but also reticence and nonacknowledgment.
According to Dr. Jordan, Edward Henry, Arlene Berry was transferred to Sunbury Regional Hospital under the care of Dr. Adegbite, a Neurosurgeon. She ultimately ended up under the care of Sauve, Stephane Jean,
ADEGBITE, Andrew B O FRCSC, Mackey Bldg., 440 - 30 Durham St., Sudbury ON P3C 5E4, Tel. (705) 673-3130, Ibadan 1976
http://www.freewebs.com/redress/Legacy.htm
http://www.freewebs.com/redress/SAUVE.htm
http://www.freewebs.com/medical_secrets/Sauve2.htm
http://www.freewebs.com/redress/Adegbite.htm
From the information at hand it seems clear that Drs. Sauve and Adegbite sought to open the way, under misleading conditions (influence of drugs, and metabolic disturbances) to organ donation from brain death. The diagnosis of brain death allows organ donation or withdrawal of life support. Certifying brain death to cover-up medical blunders or to increase organ donations constitutes murder. Alternatively, Drs. Sauv� and Adegbite merely pretended to take the deceased victim's eyes to conceal sunken eyes (sunken into orbitals), associated with a withdrawal of life support in a critically ill patient and in particular, due to severe "dehydration". The eyes turn cloudy and sink in to be level instead of rounded, which happens very soon after severe dehydration. The visual effect is indistinguishable from that associated with brain death.
A-1 of the decedent's record also documents "she died several days later with numerous metastatic lesions to her brain". According to her death certificate, Arlene Berry died May 24th of 2000, the very same day. As to the cause of death, according to Dr. Sauve in Sudbury, she died meeting "brain death" criteria. Apart from the questionable diagnosis of brain death, No pathalogical reason was given. The patient was simply hurried to her death.
The first criteria for the determination of brain death were developed in 1968 in part to address concerns that had arisen with the retrieval of organs for transplantation.
Neurolept-analgesia, which is produced by the combination of an opioid (MS Contin) and a tranquilizer (prochlorperazine), is defined as a state of CNS depression.
Picture yourself, or that of a loved one with most of your senses blunted, unable to move, speak or even open your eyes due to a severely paralyzed motor function - you try relentlessly to free yourself until you become so overwhelmed by exhaustion, fright and panic that your heart rate goes into tachycardia. That's exactly what happened to Arlene Berry. She became the victim of a horrific chain of medical negligence that is nothing short of criminal. The doctors withdrew life support, allowing her to suffocate to death before diagnosing brain death. After a loss of perfusion of perhaps 15 minutes they (the Sudbury doctors) performed a paltry CT showing a loss of cerebral perfusion due to lack of oxygen to justify reasons for her death, then shipped her off to the morgue where she remained for several days before returning her remains to Kirkland Lake, Ontario.
In the face of severe infection it seems unlikely that organ harvest could have taken place short of ALSO subjecting the recipient to high risk infection, or criminal negligence.
CAVEAT: Drug intoxication and neuromuscular blockade use are reversible causes of coma that can mimic brain death. Further, deep anesthesia (including high dose narcotics) can also mimic changes that occur with cerebral ischemia, including a loss of perfusion. All the so-called major tranquilizers can mimic a death-like condition by causing reduced brain wave activity and lack of responsiveness. Encephalopathy with peripheral neuropathy may falsely mimic brainstem death. Acute metabolic derangement and endocrine crisis can mimic brain death. Demyelinating polyradiculoneuropathy may also resemble brain death.
Brain death is defined as the irreversible cessation of function of the entire brain with three specific criteria: 1) coma, 2) absent brainstem reflexes and 3) apnea. In addition to these clinical criteria, there are important prerequisites: 1) NO intoxication or poisoning, 2) NO core temperature greater than 32 degrees Celsius, 3) clinical or neuroimaging evidence of acute central nervous system catastrophe and 4) absence of confounding medical conditions such as severe electrolyte, acid-base, or endocrine disturbances.
Most organ donors have functioning respiratory and circulatory systems.Feeling no pain; it doesn't sound like a problem, but it can be lethal for the victims of chemical restraint involving, among other things, insensitivity to pain.
Some physicians have proposed actively euthanizing comatose patients for their transplantable organs, a suggestion that is particularly disturbing in light of a British study that indicated that up to 41 percent of �permanently comatose� patients had been misdiagnosed and that some were actually awake and aware. Canadian figures would be no different.
Administering sedatives, analgesics and/or muscle relaxants to hasten death is a practice that is both illegal and unethical.
Heparin may hasten death by aggravating high intracranial pressure or promoting fata_ hemorrhage.3,5
Blood supply to vital organs is interrupted between the time of death and the removal, cooling and preservation of organs. One strategy to reduce this �warm ischemic time� and to promote organ viability is to withdraw life-support in an operating room (O.R.), where organ harvest can commence immediately.
Practices of anaesthesiologists with regard to withholding and ...
Canadian ICUs also reported an increase in withdrawal of life support from 44% to 74%. How many are actually murders???
The patient should have had a normal temperature and have been free of drugs that can suppress brain activity before a diagnosis was made on EEG or CT criteria. No autopsy was done. A subsequent request to the regional supervising coroner for a formal inquest was denied in order to prevent the truth from getting out.
Interestingly, Dr. Sauv� was a classmate of Dr. Spiller from the University of Toronto, Class of '89. It seems that Dr. Sauv�'s name apprears on a Clinical Investigator Inspection List (CLIIL) for Investigational New Drug Studies, and also on the Population Health Research Institute suggestive of perhaps some hidden agenda. He is listed in the Preceptor Handbook as the ICU contact.
Another suspect in this theft of organ from a living person is Adegbite, Andrew Babafunso Olanrewaju (CPSO#54992 ), together with an accomplice, Dr. S.Sauve (CPSO# 61381)
Guillain�Barr� syndrome mimicking brainstem death is reported in J Neurol Sci 1993; 120: 115�7.[CrossRef][ISI][Medline]
Metabolic impairment causes demyelination or axonal degeneration. Axonal degeneration secondary to severe demyelination may mimic brain death.
Brain death: resolving inconsistencies in the ethical declaration
Critical illness polyneuropathy is an ICU-acquired condition that affects the peripheral nerves, muscles, and neuromuscular junction. Neurologic crises (polyneuropathy - a reversible cause of paralysis) is associated with prolonged length of ICU and hospital stay and requirement for rehabilitation, with significant use of healthcare resources and cost implications. Neurologic crises may be the beginning of a long-lasting depressive illness followed by arreflexia and acute hypermagnesemia (after use of laxatives), resulting in hypermagnesemic pseudocoma.
"Pseudocoma" (pseudocoma: states resembling acute unconsciousness but with self-awareness preserved) of this kind may be associated with normal consciousness or relatively mild psychological disorders. Most of the cases of this syndrome are caused by basilar artery thrombosis. Further, hypermagnesemia, or hyperglycemia can mimic a variety of neurological symptoms. Many conditions can MIMIC brain death clinically upon examination and without excluding them; you will KILL a person legally despite the reversibility of brain damage. Further, drug intoxication may cause a deep physiologic depression similar to brain death.
Hypermagnesemia causes neuromuscular blockade by inhibiting the release of presynaptic acetylcholine, which results in flaccid paralysis and respiratory paralysis.
pol�y�ra�dic�u�lo�neu�rop�a�thy (p l
l
 -r
-r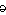 -d
-d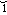 k
k y
y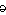 -l
-l -n
-n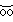 -r
-r p
p
 -th
-th )
)
| The center is filled with polymorphonuclear leukocytes and cell debris, and the outer ring is ... polyradiculoneuropathy, and diffuse CNS involvement [2]. ... linkinghub.elsevier.com/retrieve/pii/S0303846704002185 - |
eMedicine - Infectious Myositis : Article by Mohammed J Zafar, MD
|
Acute Inflammatory Demyelinating Polyradiculoneuropathy ... with an inflammatory response consisting of mononuclear and polymorphonuclear leukocytes. ... |
eMedicine - Infectious Myositis : Article by Mohammed J Zafar, MD
|
Acute Inflammatory Demyelinating Polyradiculoneuropathy ... with an inflammatory response consisting of mononuclear and polymorphonuclear leukocytes. ... |
Turning off a respirator is a form of passive euthanasia that is practiced by doctors with a family's consent. Turn off the respirator and in the natural course of affairs the patient dies of lack of oxygen (to kill or destroy by preventing access of air or oxygen). To impair the respiration of a patient is to asphyxiate, suffocate, smother (deprive of oxygen) and prevent the patient from breathing.
"To suffocate" is to die from lack of air. The term suffocation is sometimes employed synonymously with asphyxia. In the strict medico-legal sense it signifies asphyxia, caused by lack of oxigen or obstruction of the breathing passages. Asphyxia is a physiology/pathology term referring to breathing insufficiency leading to inadequate intake of oxygen and inadequate exhalation of carbon dioxide. Asphyxiation may be divided into three categories: suffocation, strangulation, and by chemicals (biochemical), ie. drugs.
Pre-euthanasia tranquilization is achieved using a combined administration of a neuroleptic (tranquilizer) such as prochlorperazine, and an opiate (analgesic) narcotic such as MS Contin to produce a form of drug-induced paralysis (analgesia), accompanied by general quiescence and psychic indifference to environmental stimuli, with altered awareness, but without actual loss of consciousnes; neuroleptanalgesia - an intense analgesic and amnesic state produced by the combination of narcotic analgesics and neuroleptic drugs.
In this case there was spontaneous muscle activity marked by short spasmodic contractions/retractions of the right leg evidenced by family. All the patient could do was wiggle her toes in response to verbal command by her spouse.Neuroleptanalgesia: An intense analgesic and amnesic state produced by the combination of narcotic analgesics (MS Contin) and neuroleptic (Stemetil/Prochlorperazine) drugs.
The administration of a combination of a narcotic analgesic and a neuroleptic agent will result in neuroleptanalgesia, with DRUG-INDUCED REDUCTION OF OXYGEN INTAKE.
suffocates - definition of suffocates
Asphyxia - Wikipedia, the free encyclopedia
View the medical record of Arlene Berry and compare.

|
Hyperglycemia and Infection in Critically Ill Patients Disorders of Acid-Base and Potassium Balance: Plasma Potassium ... Hypokalemia, with associated flaccid paralysis. eMedicine - Hypokalemia : Article by Eleanor Lederer, MD When hypokalemia is severe, it can impair respiratory muscle function, leading to hypoventilation. Most cases of acute flaccid paralysis with a preserved sensorium result from diffuse disorders of the motor unit, such as in axonal polyneuropathy or axonal demyelinating neuropathy COMPARE: West Nile virus infection in the intensive care unit: a case ... If hyperglycemia is left untreated, it can lead to an emergency condition called ketoacidosis (sometimes called DKA or diabetic ketoacidosis). |
Dr. S.Sauve (CPSO# 61381) - a co-conspirator in the Arlene Berry death coverup.
eMedicine - Hyperosmolar Hyperglycemic Nonketotic Coma
Women's Health Advisor 2005.4: High Blood Sugar (Hyperglycemia)
[DOC]
| File Format: Microsoft Word - View as HTML Case of anaesthesia of the left and of paralysis of the right side of the body. ... In catalepsy, |
http://www.freewebs.com/medical_secrets/Cisternae.htm
http://www.geocities.com/wrongful_death2000/OPINION.html
| http://ca.geocities.com/target_nova/EuthenasiaUnderground.HTM |
http://www.freewebs.com/medical_secrets/NeuroleptanalgesiaFactoid.HTM
Case in point: http://h1.ripway.com/redress/Legacy